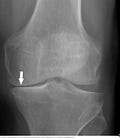
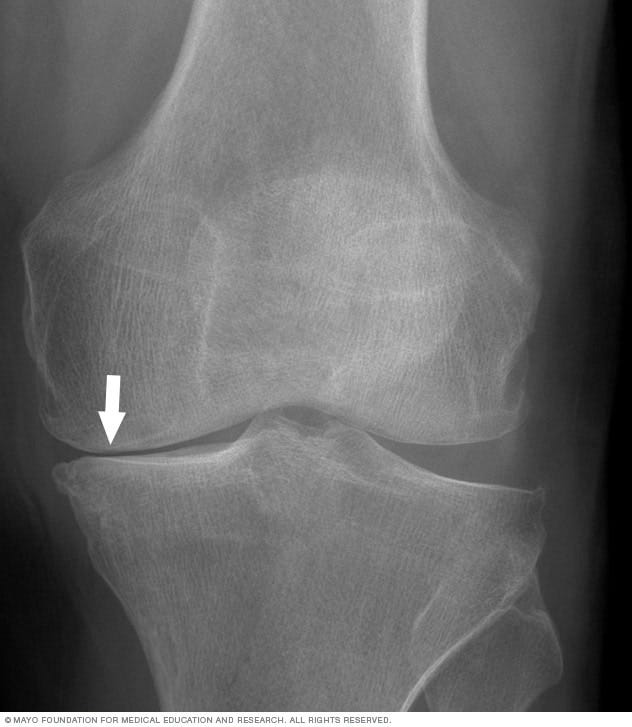
You know how sometimes when a doctor shows you your x-rays, you can’t really tell what they’re looking at? This time, even I could see it: The x-rays showed pretty clearly that I’d lost cartilage in both knees, one significantly more than the other. Osteoarthritis was the diagnosis.
Not that I was surprised. Years of high-impact aerobics and other sports, high heels on city streets and several meniscus surgeries made it pretty clear that I’d probably eventually struggle with knee pain. And aging — well, that’s another cause of osteoarthritis, along with family history. And being overweight. Ouch.
Actually, knee pain is an anodyne way of talking about something that has totally changed my life.
I have always loved sports of all kinds, but now I carefully plan what exercise I’m going to do based on how my knees are feeling. Biking, rowing, swimming and yoga — all of them as non-impact as possible — have replaced running, aerobics and even walking, though sometimes even these low-impact sports make me sore and achy (and let’s admit it: cranky) for hours afterward.
I haven’t worn my beautiful high-heeled shoes in months.
Standing is the worst, especially for long stretches. Which happens more often than I ever noticed before — at the store, during choir rehearsal, waiting for a friend to meet me for lunch.
Of course, I’m not alone: The Centers for Disease Control say that one in five US adults have some form of arthritis (there are 100 different kinds; osteoarthritis is the most common). As the population ages, more and more people will be diagnosed. It’s the third most rapidly rising condition associated with disability, behind diabetes and dementia. Many of you reading this today are surely with me on this painful journey.
But here’s the thing: I’m really trying to fight the just-give-me-a-pill solution that’s so tempting sometimes. I want to keep moving and feeling good.
It’s also become clear to me that many of my symptoms are as related to menopause as they are to arthritis. (Now there’s a sentence I never imagined sharing with the world.) The hormonal changes that menopause brings on can contribute to joint and muscle pain, not to mention crankiness and outright depression. I never had the epic hot flashes that plague some of my friends, but waking up in the night because of joint and leg pain might be just as disconcerting. Not to mention annoying — it’s hard to be at your entrepreneurial best the next day when you only sleep in two-hour increments.
Yes, I know this sounds like complaining. And I REALLY hate complaining. But I have come to realize that I may have fallen into the pattern I used to pin on my mother and some of my older friends: Everything’s fine. I’m sure I’ll feel better tomorrow. There’s probably nothing I can do.
Pardon me, but when it comes to our health, especially as women who want to stay active, keep working and remain in the world, that’s just ridiculous.
If our doctors aren’t answering our questions — or if we’re too timid to ask them — we need to make a change.
If taking OTC pain meds for the rest of your life seems to be the only solution offered to you, it’s time to find another solution.
Should I have had to read about menopause symptoms and knee pain online or worse yet, follow menopause influencers on Instagram? (Though I see a lot of you follow them, too.)
Here’s my current plan:
I have an 8-week prescription for physical therapy for my knees, and I will fully commit to doing the exercises prescribed. I’ve already started doing the three exercises every other day that the orthopedist recommended. They hurt, and I can’t see much change in my knee pain yet, but I’ll keep going. Consistency is hardest for me, but just a half-hour every day seems doable.
I also want to recommit to eating well, including leaning on the anti-inflammatory foods that have made me feel (a little) better before — whole, unprocessed foods, including lots of vegetables, and no added sugar. Green juice — a friend has a recipe that actually tastes great — has helped before. No white bread, pasta, rice. That’s a tough ask.
Mostly, though, I want to commit to asking questions, continuing to search for good information, and being patient with the process. And taking Tylenol if I really need to.
What has worked for you?



Thanks, Leanne. I hope your plan works for you, for however long. I too am beginning to feel various forms of arthritis, notably in my right middle finger, called ‘trigger finger’. This was probably brought on by years of daily cooking for lots of people. I also am dealing with many menopausal delights and navigating mostly by personal research and talking with friends and family about their experiences. I feel that I get no definitive answers from my doctor. In fact, her information often contradicts what I read from the Mayo Clinic’s. I was prescribed an antidepressant for mood swings that I am loath to take because of the possible side effects. Alas, I too am trying to eat well, exercise and meditate occasionally. Wish me luck!
Thanks Leanne for this. I recently went to a friends home for a talk about menopause. There were 25 women (58 yo - 68 yo) there to listen to a female OBGYN doing research on menopause at University of Colorado Anschutz. She spoke about how there are so few doctors doing research in this area and the very little to no training OBGYN's get on this. Because (not a surprise) there is not money in it. Money for OBGYN's is delivering babies and doing surgeries. She encouraged all of us to press our doctors to do more and keep asking questions. She said there are good results out there regarding HRT and to recognize (as you did in this) hot flashes are NOT the only menopause effect. Lack of energy, brain fog, muscle aches, joint pain and arthritis are just a few. Good luck with your plan - I too am focusing on low impact activities as I have muscle aches and joint pain. I think I need to try cutting out the white flour and sugar - sounds so hard!